Wednesday, October 22, 2014
Tracking #Ebola Effectively hindered thanks to #ICD10 (double) delay
Offers a timely reminder that the US Government delayed a second time the implementation of ICD10 coding system that is used in the rest of the world
There is no code for Ebola in ICD9 - just a non-specific 078.89: Other specified diseases due to viruses which covers:
Disease Synonyms
Acute infectious lymphocytosis
Cervical myalgia, epidemic
Disease due to Alpharetrovirus
Disease due to Alphavirus
Disease due to Arenavirus
Disease due to Betaherpesvirinae
Disease due to Birnavirus
Disease due to Coronaviridae
Disease due to Filoviridae
Disease due to Lentivirus
Disease due to Lone star virus
Disease due to Nairovirus
Disease due to Orthobunyavirus
Disease due to Parvoviridae
Disease due to Pestivirus
Disease due to Polyomaviridae
Disease due to Respirovirus
Disease due to Rotavirus
Disease due to Spumavirus
Disease due to Togaviridae
Duvenhage virus disease
Ebola virus disease
Epidemic cervical myalgia
Infectious lymphocytosis
Lassa fever
Le Dantec virus disease
Marburg virus disease
Mokola virus disease
Non-arthropod-borne viral disease associated with AIDS
Parainfluenza
Pichinde virus disease
Tacaribe virus disease
Vesicular stomatitis Alagoas virus disease
Viral encephalomyelocarditis
Applies To
Epidemic cervical myalgia
Marburg disease
ICD-10 has one specific code for Ebola: A98.4 - Ebola Virus Disease
Clinical Information
A highly fatal, acute hemorrhagic fever, clinically very similar to marburg virus disease, caused by ebolavirus, first occurring in the sudan and adjacent northwestern (what was then) zaire.
Accurate tracking and reporting stop at the border of the United States
This is one of many examples of codes "missing" in ICD9 for conditions and care we are already delivering and dealing with
Wednesday, January 22, 2014
Integrating Clinical Documentation Improvement into the Doctors Workflow
In a recent study of physician attitudes toward clinical documentation technology and processes clinicians the majority of clinicians said they would be more responsive to Clinical Documentation Improvement (CDI) clarifications if they were delivered in real-time within their normal documentation workflow in the electronic health record (EHR). They report being "disrupted" by queries for additional information
after they’ve documented in a patient chart or worse, after the patient is discharged. All believe that ICD-10 will make matters much worseWith #HealthIT a growing portion of how doctors do their jobs they want to be involved in technology decisions yet most were not involved in clinical documentation technology decisions for their organization. And timing is everything - going back to answer questions after you have left the patient or worse after the patient has left "the building".
So what is the difference between success and failure of a CDI program
As the study points out physicians’ growing dissatisfaction in being
saddled with processes that distract them from clinical care, while being excluded from the decision-making process of choosing things that impact them every dayTechnology should be simple and work for physicians and the key to changing the experience is to eliminate rework
Rework in clinical documentation is the enemy of efficiencyAs Brian Yeaman, MD CMIO for Norman Regional Health System puts it
Using things like CLU and applying that to the ICD-10 code book to help me refine that diagnosis or ask me whether it’s the left or right or an upper or lower extremity are tremendous because it has a significant impact on our bottom line, and it’s also a physician satisfier … and on the back side we are not getting so many coding queries
And Reid Conant, MD President and CEO of Conant and Associates says
“Now we can provide our physicians with tools to get real-time feedback to not only change that document, but also change their behavior for the next document. That’s what organizations are looking for, and frankly, that’s what the doctors are looking for.”
We can achieve ICD10 compliance without breaking the back of clinicians
Monday, November 4, 2013
Must we Move to ICD10 - Short Answer is Yes
For the individual doctor taking care of the patients they often see no direct benefit from ICD-10….or from SNOMED CT, LOINC, RxNorm, APR-DRG’s, ICD-9, APC’s, HCC’s, etc. But in the healthcare continuum that requires more than a single patient to be cared for and whole populations to be considered we need evidence and data to manage populations that has enough detail that has kept up with the explosion of medical knowledge. Yes capturing the codes may be difficult but the good news is there is technology to help clinicians to capture it at the point of care - anywhere and offers realtime feedback to the doctor with the unique and innovative Computer Assisted Physician Documentation (CAPD). ICD-10 is no longer to be feared but should be embraced as a bright new future that will start to code information in sufficient detail that is more representative of the complex nature of patients and their clinical condition. No longer grouped together in broad categories that do not adequately take account of the complex cases offering a much more nuanced view of the severity of illness.
So what is the difference between the two systems and what makes ICD-10 the right choice? Some of this relates to terminology and classification - nicely explained here by Dr Peter Johnson explaining the SNOMED CT system. As he says
Classification system,
A classification scheme could be thought of as a collection of buckets into which a care provider throws a particular concept or record. And since there can only be one bucket into which a concept fits, the process of labeling the buckets often leads to catch-all terms like: ‘Disease X, unspecified’ or ‘Y, not elsewhere classified’. As a result, accurately classifying records is rightly seen by most care providers as a separate process from record creation and is typically carried out by specially trained coders who know how to apply the process.
Terminology System
..a terminology allows the user to specify precisely what they want to record. Specifically, a terminology doesn’t have any ‘not elsewhere classified’ bucket terms, but is designed to have the terms that a user needs to record what actually happened.
Which brings me to the problem with SNOMED CT as a replacement for ICD-XX - clearly described by Carl Natale’s in his post: Why SNOMED cannot replace the ICD-10-CM/PCS code sets. As Carl rightly points out:
Physicians are going to have to learn how to communicate with EHRs — which will be based upon SNOMED — to comply with Meaningful Use. So the transition to SNOMED-CT already is in the works.We do need more specific documentation but as a colleague of mine has pointed out this is not the onerous task that it first appears to be - much of the data is already information we capture as part of a normal clinical interaction and the additional data requirement may only be one clinical element.
For the construct of an ICD-10 code we have 7 characters made up as follows
- Section,
- Body System,
- Root Operation,
- Body Part,
- Approach,
- Device,
- Qualifier
Open reduction internal fixation distal phalanx right index finger with K wire
contains everything necessary to code this as
0PST04Z - which is made up of:
- 0 - Medical Surgical
- P - Upper Bones
- S - Reposition
- T - Finger Phalanx R
- 0 - Open
- 4 - Internal Fixation Device
- Z - No Qualifier
Basically, ICD-10 codes aren't the problem. It's the specificity of documentation that will be required one way or another. SNOMED should make it easier to document to the required specificity. It is then up to the EHR system to convert that data to ICD information. Hopefully the physicians won't know what level of ICD is being used. They will just need to know what needs to be recorded.So what does this look like in the clinical setting - this video offers a peek into the new world of documentation and how Healthcare technology, Clinical Language Understanding and integrated solutions will start to ease the documentation burden, allowing clinicians to focus on care and the patient and not documentation coding
Monday, November 26, 2012
ICD-10 and Its Impact on Radiology
December 2011
ICD-10 and Its Impact on Radiology
By Ronald V. Bucci, PhD
Radiology Today
Vol. 12 No. 12 P. 10Dr Jones sends his patient John to the radiology department for an x-ray of his nasal bones. John’s pet turtle bit him and, distracted by the pain, John walked into the lamppost in the driveway of his mobile home, causing him to break his nose and develop a headache.1
In the coming world of ICD-10, we’ll actually have—perhaps unbelievably—several ICD-10 codes in play for a case such as this one: W59.21XA, Bitten by turtle, initial encounter; W22.02, Walked into lamppost; Y92.024, Driveway of mobile home as the place of occurrence of the external cause; S02.2, Fracture of nasal bones; and G44.311, Acute posttraumatic headache intractable.
The upcoming transition to ICD-10 on October 1, 2013, and the new electronic transactions standards for claims that go into effect on January 1, 2012, grew out of HIPAA. The law included provisions for the standardization of healthcare information, designating standards for transactions of medical information, including claims, eligibility, and referral authorizations. On January 1, 2012, the electronic transaction standard for claims submission will change from version 4010 to 5010. On an even larger scope, the 2013 conversion from ICD-9 codes to ICD-10 codes will dramatically change the revenue cycle for all healthcare institutions. Together, version 5010 and the ICD-10 code adoptions are the solution to standardized healthcare information for HIPAA compliance.
ICD-9 codes have been around for approximately 30 years, and version 4010 has been the electronic transmission standard since the inception of electronic claims. The ICD-9 codes are used in medical billing and are the diagnosis codes for a patient’s medical conditions. A typical code might be 782.3 for edema or 486 for pneumonia. ICD-9 is the official system used to assign codes to diagnosis procedures for patient treatment in all settings. The ICD-9 codes are three to five alphanumeric characters, and there are approximately 18,000 such codes in the system. The current ICD-9 codes present some challenges. Some use outdated and obsolete terminology, lack detail, are not applicable to today's practice of medicine, and do not fit in with the HIPAA provisions.
ICD-10 will be introduced with some significant differences from ICD-9 codes. There are two types of ICD-10 codes: ICD-10-CM and ICD-10-PCS. ICD-10-CM is the diagnosis classification developed by the Centers for Disease Control and Prevention for use in all U.S. healthcare treatment settings. These codes have three to seven alphanumerics and are very similar to the ICD-9 codes. There are approximately 68,000 of these codes. ICD-10-PCS is a procedure classification system developed by the Centers for Medicare & Medicaid Services (CMS) for only U.S. inpatient hospital settings. These codes use seven alphanumeric characters, and there are approximately 72,000 of these codes. Under ICD-9 when you see a given CPT code, you can usually identify the appropriate diagnostic code from a short list of candidates. With ICD-10 codes, this number of diagnostic codes increases by nearly tenfold.
Similarities and Differences
There are some similarities and many differences between the old and the new diagnosis codes, including more characters and codes in the ICD-10 system. The main differences between ICD-9 and ICD-10 codes are shown in Figure 1.2The CMS believes the change from ICD-9 to ICD-10 will bring improvements and benefits to patients, medical institutions, businesses, and the government. Some of the anticipated benefits are shown in Figure 2.2
ICD-10 codes were designed to be more specific than ICD-9 codes. The new codes will have details such as left or right body parts, the exact location of the condition, the activity during the initial or a subsequential encounter, and whether episodes are acute or chronic. For example, if someone fell on the ice while skating and suffered a concussion, the medical facility would have to report multiple ICD-10 codes for the occurrence: the concussion, the external cause (ice), the activity (skating), the location (where the ice rink is), and whether the injury was acute or chronic. Specific components incorporated into the new codes include the following:2
• laterality (left, right, bilateral);
• combination codes for certain conditions and common associated symptoms and manifestations;
• combination codes for poisonings and their associated external cause;
• obstetric codes identify trimester instead of episode of care;
• character “x” is used as a fifth character placeholder in certain six-character codes to allow for future expansion and to fill in other empty characters (eg, character 5 and/or 6) when a code that is less than six characters in length requires a seventh character;
• two types of Excludes notes: one for codes and one for conditions excluded;
• inclusion of clinical concepts that do not exist in ICD-9-CM (eg, underdosing, blood type, blood alcohol level);
• numerous codes have been significantly expanded (eg, injuries, diabetes, substance abuse, postoperative complications); and
• codes for postoperative complications have been expanded and a distinction made between intraoperative complications and postprocedural disorders.
With these new codes, the inventory of diagnosis codes will increase from 18,000 to 140,000. While there may have been one code for a particular occurrence in the ICD-9 list, there may be 10 or more ICD-10 codes. For example, in the old system, there was one code for angioplasty; in ICD-10, there are approximately 854 codes. In ICD-10, there are 195 codes for suturing an artery and 312 codes that involve animals, with 72 of those dealing with birds.2 Of the 140,000 new codes that will be available, some are unique and interesting, such as the following:
• W61.42, Struck by turkey, or W61.43, Pecked by turkey;
• S45.911, Laceration of unspecified blood vessel at shoulder and upper arm level, right arm;
• S91.232, Puncture wound without foreign body of left great toe with damage to nail;
• R46.0, Very low level of personal hygiene;
• T71.233, Asphyxiation due to being trapped in a (discarded) refrigerator, assault;
• Y92.65, Oil rig as the place of occurrence of the external cause;
• T43.612, Poisoning by caffeine, intentional self-harm; and
• V04.09, Pedestrian on snow skis injured in collision with heavy transport vehicle or bus in nontraffic accident.
Impact on Radiology
Radiologists depend on the referring physician to give the order for and the reason behind an exam. They are also dependent on the physician for pertinent information related to an ordered exam. With ICD-10 codes, the amount of information required from the referring physician increases dramatically. Imaging facilities will have to acquire a much greater history for a patient when scheduling an exam for the purposes of precertification, dictation, and subsequent billing of a procedure.Secondly, radiologists must be much more specific and detailed in their documentation and wording of a completed exam. The coding of the dictation will depend on whether the patient is an inpatient or an outpatient, since ICD-10-PCS codes are only for inpatient procedures. Therefore, the same patient can have the same exam twice, one as an inpatient and one as an outpatient, and the report codes will not be equivocal. In the ICD-10-PCS codes, there are three sections devoted to radiology. Radiologists will need to pinpoint the areas being imaged and the type of imaging being performed.3
ICD-10-PCS codes for inpatients must be matched correctly with the CPT code for the procedure. For example, suppose a patient fell in a chicken coop, suffered significant head trauma, and was admitted to the hospital. The patient was then sent for an MRI of the brain. Under the current system, the billing department would use CPT code 70551 for an MRI of the brain without contrast. The matching ICD-10-PCS code is B030ZZZ, Magnetic Resonance Imaging (MRI) of Brain. It would also be necessary to match up codes for the diagnosis in the ICD-10-CM code list, including S06.0X1A, Concussion with loss of consciousness of 30 minutes or less, initial encounter, and Y92.72, Chicken coop as the place of occurrence of the external cause.
Failure to include the appropriate codes and detailed reporting will delay reimbursement and possibly cause a loss of revenue. The challenge for radiology providers will be preventing referring physician offices from inhibiting their work because the referrers are not ready for the new codes and reporting requirements. Imaging facility managers will need to work closely with referring physicians and help them prepare for the ICD-10 introduction on which radiology’s billing depends.
Getting Ready
It is imperative that radiology providers start planning now for the October 2013 implementation. Facilities need to develop a strategic plan to make the conversion to the new system, perform training, and then test the training. Some suggestions for how to get ready include the following:• Become familiar with the CMS website for ICD-10 (www.cms.gov/ICD10).
• Perform a SWOT (strengths, weaknesses, opportunities, threats) analysis in your department on the basis of the current state of employees, IT, and environment.
• Determine your department’s future statement (what you intend to achieve) for ICD-10 implementation.
• Form a strategic business plan detailing the strategy to move to the future statement.
• Gain buy-in from management.
• Implement your strategy.
• Test, measure for successes and failures, and always improve.
A few other key points and suggestions:
• All personnel, systems, and functions in the radiology revenue cycle process should be involved in this process, from patient registration to delivering the radiology report to subsequent billing of the procedure.
• Identify challenges, including an understanding of the timeline associated with and implementation of the new codes, communication throughout your departments, IT, educating everyone in the department, and expected dysfunctions inherent to your institution.
• Develop education/training plans for all employees.
• Send radiology schedulers to medical coding classes or “boot camps” and require them to get certified in medical coding. It would be beneficial for your schedulers to know what information is needed when they schedule appointments and obtain detailed information at the first intake level.
• Enable your radiologists to go through training for dictation specifications.
• Work with referring physicians to make sure they are preparing for the ICD-10 transition and offer help to them.4
Final Thoughts
Though October 1, 2013, may seem far away now, it will be here sooner than you think. Now is the time to prepare for potential coding challenges related to the changes, which will have huge implications on the radiology revenue cycle. There is much to lose in the way of revenue if a radiology department is not ready for the new codes. If you take the time now to properly prepare and train your employees for the changes, then you will be able to take advantage of the benefits of these new codes and not interrupt your business and the financial stream that supplies your institution.— Ronald V. Bucci, PhD, is administrative director of radiology at Akron Children’s Hospital in Ohio.
Figure 1
Comparing ICD-9 TO ICD-10ICD-9-CM Diagnosis Codes
• Three to five characters
• First character is numeric or alpha (E or V)
• Characters 2 through 5 are numeric
• A decimal is used after three charactersICD-9-CM Procedure Codes
• Three to five characters
• All characters are numericICD-10-CM Diagnosis Codes
• Three to seven characters
• Character 1 is alpha
• Character 2 is numeric
• Characters 3 through 7 are alpha or numeric
• A decimal is used after three characters
• Use of dummy placeholder “X”
• Alpha characters are not case sensitiveICD-10-PCS Diagnosis Codes
• Seven characters
• Characters are either alpha or numeric
Figure 2
ICD-10-CM Objectives
According to the Centers for Medicare & Medicaid Services, the up-to-date classifications in ICD-10 will provide much better data for the following:• measuring the quality, safety, and efficacy of care;
• designing payment systems and processing claims for reimbursement;
• conducting research, epidemiological studies, and clinical trials;
• setting health policy;
• operational and strategic planning and designing of healthcare delivery systems;
• monitoring resource utilization;
• improving clinical, financial, and administrative performance;
• preventing and detecting healthcare fraud and abuse; and
• tracking public health and risk.
Resources
• “ICD-10: Acute Myocardial Infarction” by Melody Mulaik (Radiology Management, July/August 2011)• “ICD-10 for Radiology Coding, Part 2” by Deborah Neville. (ADVANCE for Imaging & Radiation Oncology, August 31, 2011)
• “ICD-10: The History, the Impact, and the Keys to Success,” a white paper by AAPC
• “Your ICD-10 To-Do List” by John Morrissey (H&HN Hospital & Health Networks, September 2011)
References
1. Mathews AW. Walked into a lamppost? Hurt while crocheting? Help is on the way. Wall Street Journal. September 13, 2011. Available at: http://online.wsj.com/article/SB10001424053111904103404576560742746021106.html2. Centers for Medicare & Medicaid Services. 2012 ICD-10-PCS and GEMs. Available at: http://www.cms.gov/ICD10/11b15_2012_ICD10PCS.asp#TopOfPage
3. Neville D. ICD-10: Timing is everything. ADVANCE for Imaging & Radiation Oncology. May 2, 2011. Available at: http://imaging-radiation-oncology.advanceweb.com/Features/Articles/ICD-10-Timing-is-Everything.aspx
4. Hardy K. Preparing radiology for ICD-10. Radiology Today Digital Supplement. October 2010. Available at: http://viewer.zmags.com/publications/9ce7ed6e#/9ce7ed6e/4
ICD10 will be impacting radiology like many other parts of the healthcare system. In short:
- more detail on patients from the order that will be required for precertification, dictation, and subsequent billing of a procedure
- Radiologists will have to be more detailed in their documentation of exam reports
- Since ICD-10-PCS codes are for inpatient procedures only a patient can have the same exam twice
- ICD10-PCS codes will need to be matched correctly to the CPT codes and contain sufficient details
- Referring clinicians may be the source of significant challenges in your compliance if they don't include the new codes in their referrals
As the author points out - there is much to loose (information and revenue) in radiology. The time to focus is now
Monday, October 29, 2012
November Voice of the Doctor Guests
An exciting month for Voice of the Doctor with the following guests appearing
November 2: Terri Mitchell, MSN RN
Director, Clinical Informatics Solutions at Nuance Communications
We will be talking about The Healthcare Data Imperative and the challenge of capturing Healthcare data and the importance of capturing information at the point of care when the information is fresh in the mind and the value this brings to affecting a postive change in healthcare quality outcomes and appropriate reimbursement. We will discuss the need to focus on real time vs retrospective analysis and how this can be achieved in our new digital world of electronic medical records and the value of patient engagement as part of this process.
November 9: Dr Ashish Jha, MD
The C. Boyden Gray Associate Professor of Health Policy and Management at the Harvard School of Public Health and blogs at An Ounce of Evidence
He wrote this piece: Asking the Wrong Questions About the Electronic Health Record that was a response to the article posted recently on the Wall Street Journal: A Major Glitch for Digitized Health-Care Records that stated:
Now, a comprehensive evaluation of the scientific literature has confirmed what many researchers suspected: The savings claimed by government agencies and vendors of health IT are little more than hype.
And was subject to many active discussions on several of the listservs. Dr Ashish Jha and I will be discussing some of the fundamental issues of our broken system and the challenges faced in our archaic paper based system which most can agree do nothing to empower clincians to provide excellent care. Technology on its own cannot provide all the answers but must be part of a broader based solution.
The problem is that some Health IT boosters over-hyped EHRs. They argued that simply installing EHRs will transform healthcare, improve quality, save money, solve the national debt crisis, and bring about world peace. We are shocked to discover it hasn’t happened – and it won’t in the current healthcare system.
We need to leverage the potential by asking and answering other related questions
- How do we create incentives in the marketplace that reward physicians who are high quality?
- How do we allow physicians to capture efficiency gains?
- What to do about fee for service - are ACO's the answer?
- How does technology play an effective part in this transformation
As Dr Jha said:
The debate over whether we should have EHRs is over. Can we fix our broken healthcare system without a robust electronic health information infrastructure? We can’t. Instead of re-litigating that, we need to spend the next five years figuring out how to use EHRs to help us solve the big problems in healthcare.
Should be a great discussion
And to close out November I am excited to announce that I will be joined by Dr Eric Topol, MD
November 16, Dr Eric Topol, MD
Professor of Genomics at The Scripps Research Institute
Follow him on twitter @EricTopol
He is also the author ofThe Creative Destruction of Medicine: How the Digital Revolution Will Create Better Health Care and has named in the list of the Top 100 Most Influential Physician Executive in Healthcare, 2012 by Modern Healthcare
If you have not read the book, you should. You can read the First Chapter here: The Digital Landscape: Cultivating a Data-Driven, Participatory Culture to get a taste for the wide open opportunites many of which are here and even more coming in the very near future. With so many topics to choose from:
- The Current state of medicine and the challenges
- Individualized medicine vs Group Thinking
- Patient Engagement and the power of mobile Health technology
- The Genome and Sequencing (Dr Topol recently had his genome sequenced - one of an expanding number of people to do so):
We've got our genomes sequenced, now zooming in on them bit.ly/OWh6eW @illumina w/ @gholsonlyon @bradpatay
— Eric Topol (@EricTopol) October 22, 2012
And Posted some initial analysis with a 99c App!
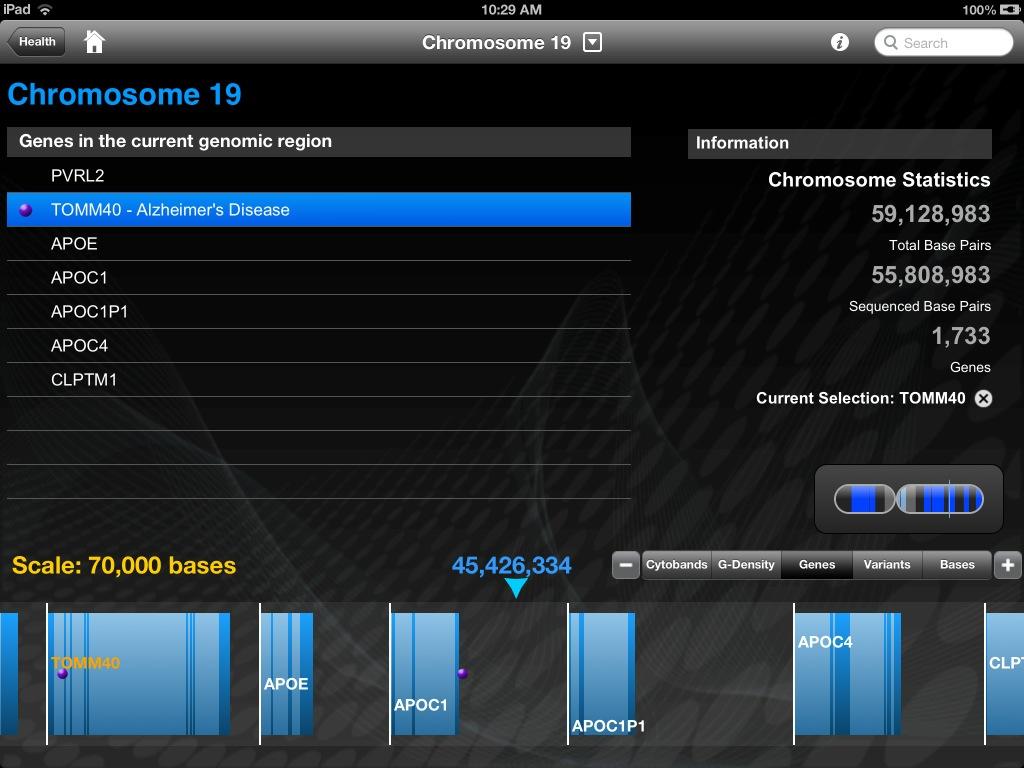
So many topics and so little time. Focusing on the current challenges in Alzheimer's treatment makes much of this come into focus. A recent story on NPR: Treatment For Alzheimer's Should Start Years Before Disease Sets In raises one of the big challenges in this disease....How do we know if we need to commence treatment for a disease. It seems unlikley that any preventative treatment can be given to everyone so identyfying those at risk will become a major focus in the coming years. As Dr Topol noted in his book and in many of his presentations and discussions on the effectiveness of Plavix varies based on presentation of the genotype CYP2C19. This was subject to an extensive debate and included this posting on the Topolog posting An important miscue in clopidogrel pharmacogenomics and in a perfect example of the use of technology and engagement this videoif this works here otherwise download a verion here)
Since November 23 is the day after Thanksgiving we will have a re-run on November 23 and Nov 30 from a previous shows
Hope you can join me
Join me on Friday at 2:30 ET on VoiceoftheDoctor
